An LVAD, a Left Ventricular Assist Device, also known as the artificial heart, is attached to the patient's heart for the purpose of pumping blood through their body. The patient's heart is in a condition that can no longer pump blood itself. There are strick requirements to qualify for an LVAD. One is that the patient must first qualify for a heart transplant. Another is the patient must be in severe end-stage heart failure.
This page is not intended to be used for detailed technical information. I would like to clarify that I am writing this casually from my experience. If you require technical information, please go to Thoratec.
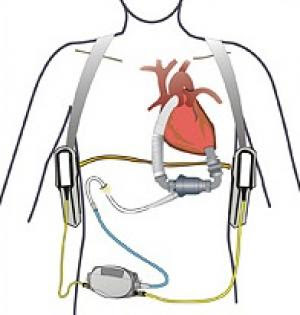
As shown below, the LVAD connects to the base of the left side of the heart and also to the aortic valve. The blood is detoured this way and then circulated through the body. The pump is very quiet. Is it continuous flow, not a pump at all really. I hardly have a pulse and a blood pressure. It's difficult to read vitals on me. An EKG is very disturbed and doesn't look like an EKG at all. But somehow, the doctors know what to look for and monitor me very carefully.
The percutaneous lead, also known as the drive line, is connect at one end to the LVAD inside of me, exits my skin and connects to the controller. The controller is the brain of the pump, if you will. It records my numbers, such as speed, flow, etc. and alerts me if anything occurs that I should be aware of. Such a case would be when the batteries are low, when the drive line is disconnected, when the controller is not functioning properly or the pump stops. The power source connects to the controller. I can have three different sources of power. One, batteries; two, the Power Base Unit (PBU); and three, the back-up battery. The batteries are mobil so I am on them all day. They actually last the whole day for me, about 15 hours. I'm connected to the the PBU at night because the alarms are much louder and would wake me up if something was to go wrong. It is plugged into the wall and has a monitor with my numbers. The back-up battery is an additional power source in case of an emergency. This could occur if the power went out, I didn't have any charged batteries AND I couldn't drive anywhere to get power from a generator elsewhere. I would like to think this would never happen but I have it just in case.
How do I carry everything, you ask?
Well, I have bags from practical to stylish! My most popular, and by far most practical, is my MEC backpack. It's actually a water pack for athletes so it's very sleek and light. I can be hands free and I often forget I have it on. It has nice support, which is a benefit because I where it just about all the time. I can fit all of my equipment into a couple of stylish purses, as well. You would never know that I'm supported by such an important, life-saving device. Some people choose to wear the holsters and others choose to wear a fanny pack. It is a personal decision.
Since anything could potentially go wrong at any time, I am required to carry my spare parts at all times. I have a few means of doing this as well. When Shaun was with me for the first few months he would carry my parts in his back pack. It made me feel better because I wasn't the only one. Now, since I am getting out without him I have a small suitcase on wheels. In this bag I must carry spare batteries, a spare controller, a spare clip, a spare alarm battery, dressing materials (in case I spill on the drive line exit site) and emergency contact numbers. If I want to get out for a walk I use my school backpack and put my connected parts as well as my spare parts in the one bag. This makes for additional exercise!
My doctor was kind enough to send me a copy of my xray. I found it incredibly interesting so I thought I would share it. There is a cloudy part that everything is connected to, that's my heart. You can see the details of the LVAD, my ICD (Ivan) and the wires along my sternum. There is ALOT going on in there. Metal detectors would scream at me!
There are some limitations I must remember while supported by the LVAD. I must avoid any significant static shock, ie. vacuuming rugs, touching tv screens. I cannot swim or be immersed in any water. I have a shower bag that is particularly designed for the LVAD. I cannot jump since the LVAD could disconnect from my heart. I cannot be in a car seat that has airbags. If they were to fire it could also disconnect the pump. I cannot have an MRI, which was also considered when I had Ivan implanted. The settings of Ivan cannot be changed because it interferes with the LVAD. I cannot sleep or lie on my stomach because of the drive line exit site. It seems like a lot but really I just get used to not doing particular things and forget about it.
What does it feel like inside you?
Another good question. At first, it hurt like words I cannot type here. I am smaller than the average patient and the LVAD barely fit in. For a good three months or so I was in constant pain. It would rub against my ribs and I would feel it's weight shift whenever I moved. Other pain would be associated with having open-heart surgery. For a while now, I have been off all pain killers and I really don't feel any pain. I honestly forget about the device and just go on living. That's the goal, right? I am very sensitive to anybody going near my abdomin, though. As you can see from the xray, there is reason to protect it.
I feel the humming if I put my hand over the LVAD and I can hear the humming when I don't have a shirt on. I often don't notice. I think I'm merely desensitized to the device. It's just the way it is.
How do you handle it emotionally?
To keep it simple, I really try not to think about the difficult things and take advantage of living. I feel great and I want to enjoy it. I am battery-powered. And I am proud to be given a second chance at living. I want to make the most out of this opportunity. If I go tomorrow, I don't want to be remembered for the things I complain about, I want to be remembered for the difference I made.
It does suck, don't get me wrong. But there is nothing I can do to the change it. I only have the power to change what's next. And so I embrace all that I can, tell those close to me that I love them, and just keep going. What would you do?






















What a coincidence! My best friend, also named Andrea (who has had two heart transplants)and just got an LVAD on Tuesday! So nice to read your story! I'm sending your link to her parents. I started a blog for her couple of months back, andreafroes.blogspot.com. Love it if you would check it out!
ReplyDeleteThanks for all the good info,
Natalie
You are truly an inspiration. I received my LVAD on 12/9/2010. It has been the most life-altering event ever and I am in constant prayer for strength, patience, and courage. Minimal exercise is taxing, but I persevere. I pray for the day of a transplant. You give me so much hope Andrea. GOD BLESS YOU!
ReplyDeleteHello Andrea,
ReplyDeleteMy name is Ann I just received my LVAD about 8 weeks ago. Could you please tell me exactly which MEC bag you chose, I have been trying to find ways to carry my controller and batteries in a more comfortable (and stylish) way. Thanks in advance and keep posting to this inspiring blog. You are a true inspiration to us all.
Hi Ann! Thanks for the comment! You got your LVAD 8 weeks ago? Wow. I have been asked about my MEC bag many times. You may know this, MEC is Mountain Equipment Coop. I got it from the MEC store in Toronto. Actually, my husband and Dad went there while I was in hospital and bought about 6 bags for me to test. I chose this one because it's sleek and has great support. The back is thick so the jagged edges didn't dig into my back. It's actually a water pack, if that helps. I believe it's the 2009 model and I haven't seen it in the store since we bought it... There are newer versions though. I just love it. I actually wore it the other day at a walk and it felt homey... I wish you the best in your recovery! You can send me an email at sa.clegg@hotmail.com if you want to chat more! I would love to know where you are from and how you are doing.
ReplyDeleteWhat a great way to tell others about life with an LVAD. I had mine implanted 3 months ago and could feel the difference right away. I get a little freaked out when I spend too much time thinking about my blood being pumped by a couple of batteries but most of the time I forget I even have the VAD. There are times when I am out and about and I forget to check the level of my batteries but I always have the spares with me. I can once again take my dog for walks of several blocks and not just the half a block I was walking before the surgery. I am now waiting for a transplant. I do have to admit it will be nice to get rid of all the wires and the pacemaker...not to fond of getting shocked but it has kept me alive for 3 years now.
ReplyDeleteGod bless you and may you have a long and fruitful life. Ron